


Patients were excluded if any of the following parameters were coded as unknown: clinical T or N stage, pathologic surgical margin status, tumor grade, estrogen receptor ER and progesterone receptor PR status, receipt of any treatment variables radiation, chemotherapy, or hormone therapy , or if it was unknown whether a DCIS component was present using the CS Site-Specific Factor 6 variable within the NCDB participant user file. At first, these changes stimulate cell growth, resulting in ductal hyperplasia an overabundance of normal cells , which may begin to fill the duct. But just to be safe patients, need to know their options, and so the radiologist does the diagnosis, and then they send the patients to the surgeon to have that discussion in greater detail. UK guidelines say that everyone who has had treatment for early breast cancer should have a copy of a written care plan. After lumpectomy Lumpectomy for DCIS is usually followed by whole breast radiation therapy to lower the risk of [ ]: DCIS recurrence a return of DCIS Invasive breast cancer A meta-analysis that combined the results of 4 randomized clinical trials showed lumpectomy plus whole breast radiation therapy lowered the risk of invasive breast cancer after DCIS in the same breast as the DCIS by 50 percent compared to lumpectomy alone [ 3 ]. It remains unclear, however, whether survival outcomes are similar for IDC when it presents alone or is accompanied by co-existing DCIS. And so I think the safe thing to say is that surgery relatively is safe, and so if we can, and it's easy for these patients, then we should be taking this area out until we get literature that suggests otherwise.
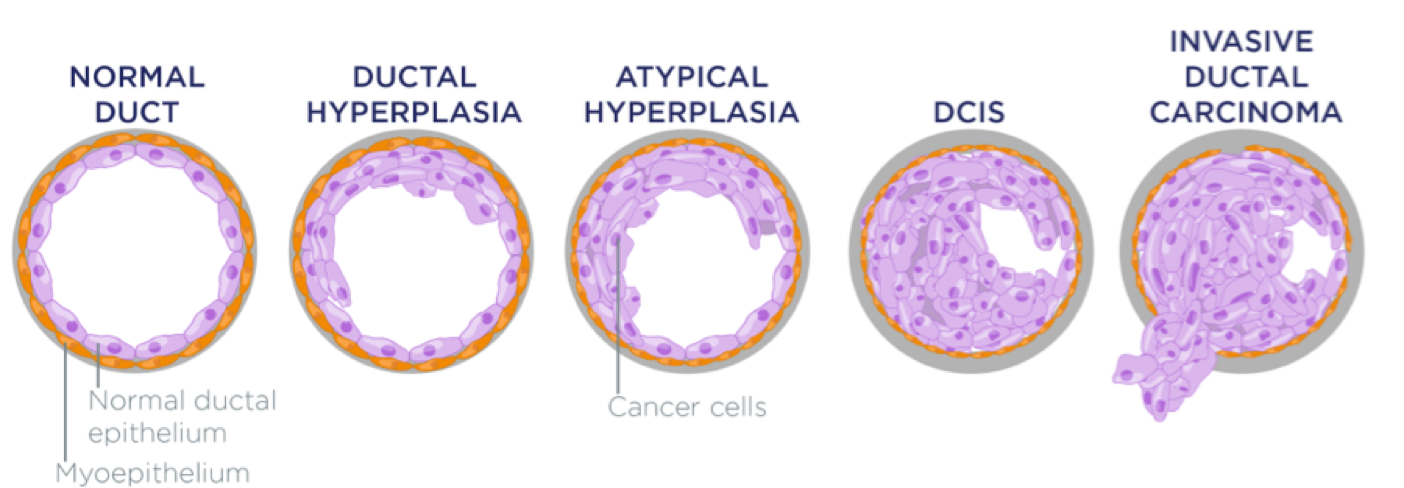
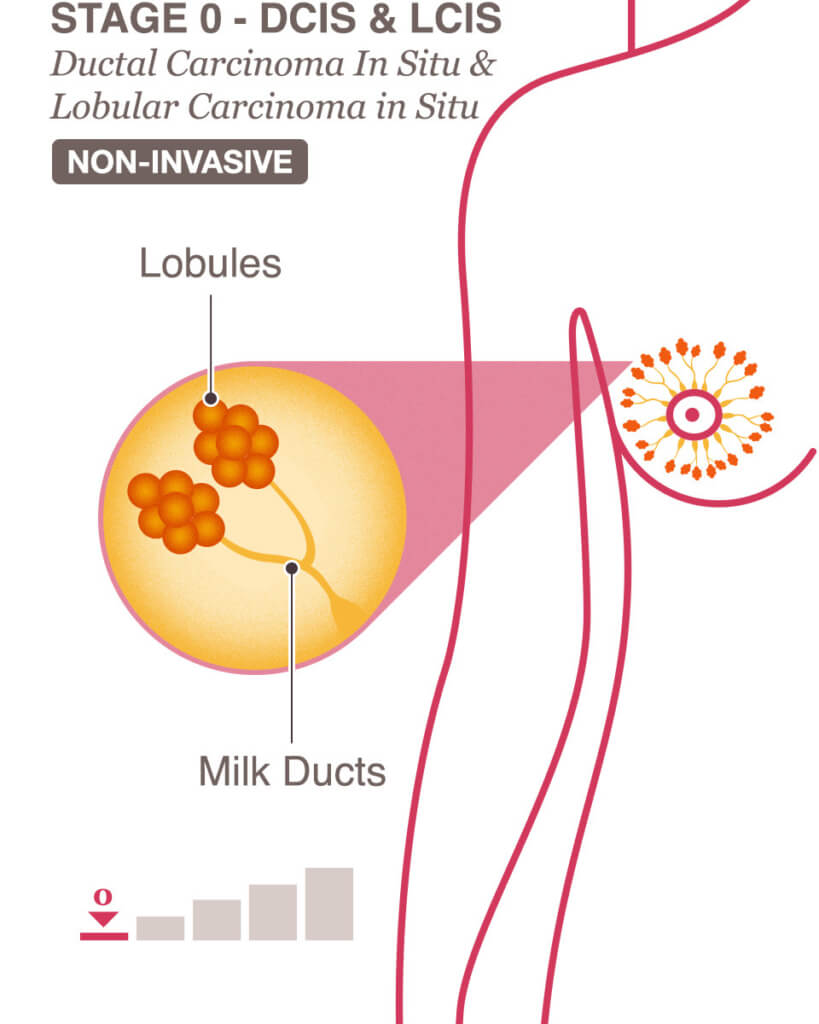


That's ClevelandClinic. Espina V, Liotta LA. The chances an area of DCIS contains invasive cancer goes up with tumor size and how fast the cancer is growing. There is a growing interest to identify patient populations for which breast cancer treatment can be de-intensified. Is it a continuous pathway? And so what the radiologist will do is a minimally invasive procedure called a core needle biopsy, and they'll either do that using mammogram guidance called a stereotactic biopsy or under ultrasound guidance called an ultrasound-guided biopsy.